The convoluted, corrupted healthcare system inherited by the Trump administration resulted from years of flawed healthcare policy and unintended consequences that put layers of bureaucrats and corporate middlemen in between patients and their medical care. The patient–physician relationship was replaced by a government-corporate insurance complex so expensive and cumbersome that patients can’t afford it or access it. Trillions of dollars are spent sustaining a dysfunctional system of bureaucrats, middlemen, and their money games while a fraction is spent on actual patients and their care.
We must understand what blew up the healthcare system, so we won’t repeat mistakes of the past as we rebuild an honest, agile, and unencumbered system. Nothing illustrates where we are and where we must go better than these two diagrams:
Diagram One
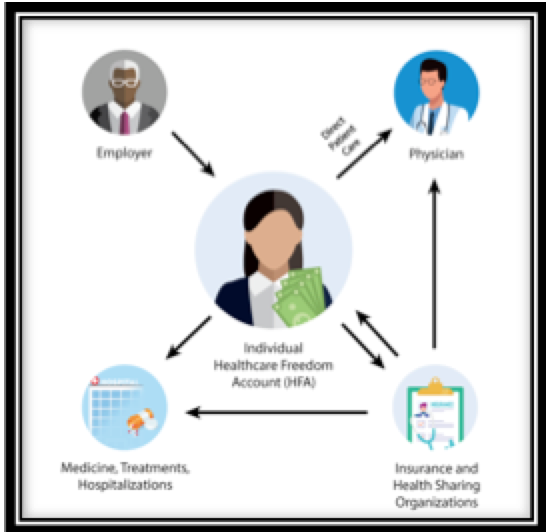
Diagram Two
The current healthcare system consists of employer-based commercial insurance (run by corporations with government strings), Medicare (run by federal government with corporate strings), Medicaid (run by the states with federal government and corporate strings), the Veterans Administration and Military healthcare Systems (run by federal government), and the Affordable Care Act (ACA) (federal ropes, corporate cords, and state strings). Diagram one represents the Affordable Care Act (ACA) as designed and implemented by the Democrats. The entire flow chart centers on an all-powerful federal government bureaucrat. A small yellow star at the very bottom in the right corner represents American patients. A small yellow cross at the very bottom in the far left corner represents physicians. This representation says it all. Sadly, the intervening bureaucrats and middlemen are feeding and multiplying unchecked.
In 2017 alone, U.S. insurers and providers spent more than $800 Billion on administrative costs of the current gluttonous system. That’s more than $2500 per person spent on bureaucracy and administration, not patient care- a far cry from the $2500 savings ACA cheerleaders falsely promised in 2010. On top of the $800 Billion is at least $250 Billion that goes to middlemen, such as pharmaceutical benefits managers (PBMs), who bilk the system via a supply chain corrupted by kickbacks called rebates and a massive pay-to-play scheme, under cover of secret contracts and loopholes created by flawed law. Collateral damage is increased drug costs, drug shortages, and tainted drugs to name a few. The common theme is, the money does not go to patients or their care.
The money goes to bureaucrats and middlemen. Because they have the money, they can make the decisions. If PBMs spend just 10% of their $250B annual bounty on lobbying and influencing elections, that $25 Billion swings a lot of weight influencing politicians and policy makers. They can get politicians elected who are willing play along, or they can bring them down, plugging in someone else willing to play by their rules. Imagine if this trillion dollars plus was actually spent on patients each year instead of entrenched bureaucrats, greedy middlemen, and manipulated politicians.
That brings us to Diagram Two. This is what we must build as we rise up and rebuild a sleek, personalized system 100% centered on the patient who controls the dollars and makes the decisions. No one will be left out, because the money and power flows through the patients. Yes, there will be a compassionate safety net too, funded by rerouting what is currently misused to actual care of those who need it most. Patients and families will control this safety net backstop, and there should be a role for true charity.
This rebuild starts with a foundation built on patients, the patient-physician relationship, and free market competition. This starts with transparency. Exposing the money games will empower patients and disempower middlemen, who will have to serve patients over themselves in an ethical fashion if they want to stay in business. Because patients control the money and decision making, they will shop around for what they deem the best cost and best care. Unshackled by government and middlemen, insurance companies will create more choices that can be personalized for each patient’s needs instead of big corporate profit.
Competition for patients’ business will bring costs down. You choose your plan, you own your plan, and you get the tax benefits of your plan and healthcare expenses, just like employers do. This way no matter what happens in your life, if you change jobs, move, or suffer a medical catastrophe, you don’t lose your plan. This will decrease administrative costs and the number of patients left in a gap without insurance, exposed to the pitfall of being classified as having a “pre-existing condition.“ Best of all, if you are blessed to have a healthy year with minimal healthcare expenses, you keep your unspent money in a personalized health savings account that can grow throughout your lifetime.
In the current system, you pay onerous premiums, end up paying out of pocket anyway, because deductibles and copays are so high, and then have nothing to show for it at year’s end. This makes the risk of going without coverage really appealing. In a new personalized system, if you don’t use the money, you keep it. Your savings from year to year will build up to a sizeable pot of money to use even as you enter Medicare age to make personal decisions about your plan, your care, and even long-term care with your dollars. As this new system progresses, if you are blessed to have money left in your account when you pass, potentially you could pass this on to your children and grandchildren for their health savings accounts. Over time, the old system will phase out under the successes of the new. Costs will come down on all aspects of your care from medications to hospitalization and surgery. Politicians will have to answer to patients not middlemen and bureaucrats.
Democrats, led by Presidential candidate former Vice-President Joe Biden and Vice-Presidential candidate Senator Kamala Harris, want to preserve the status quo and build more of the same on top of the collapsing foundation. Sadly, under this system premiums on the individual market have doubled, even tripled since ACA regulations took effect. Seema Verma, head of the Centers for Medicare and Medicaid Services (CMS), points out, “This means for a 60 year old couple living in Grand Island, Nebraska who earns $70,000 a year, the lowest cost silver plan would cost $38,000 a year in premiums with an $11,000 deductible…more than 2/3 of their income.” Americans can’t afford this. People are fleeing the market. Thus, the ACA created a whole new group of uninsured, and thereby, a new group of patients with pre-existing conditions; both groups are growing. The lie of “If you like your doctor, you can keep your doctor; if you like your plan, you can keep your plan…” has been exposed in real-time. Biden wants to lower Medicare age to 60, adding millions more to the corrupted, imploding system, while Harris wants to add a public option- another elaborate government program like Diagram One- doubling down on the waste and shenanigans of bureaucrats, middlemen, and politicians.
Republicans, led by President Donald Trump and Vice President Mike Pence, want to put American patients first and at the center like Diagram Two- personalized care for you- your money, your plan, your choice. They want patients to have Better Care, More Choice, Lower Costs. They want to get rid of the administrative boondoggle and corrupt supply chains that harm patients. They want to return the trillion dollars spent on bureaucracy each year to patients and their care. They have done all they can through decreasing regulatory burden and issuing Executive orders.
Your vote for President is critical, and so is your vote for your Senator, Representative, and state and local leaders, who will be charged with codifying each building block of the streamlined legislative structure while cleaning up the legislative rubble. Congressman Chip Roy (TX-21) understood this healthcare crisis from the beginning and introduced both the Personalized Healthcare Act (Senator Ted Cruz has a companion bill in the Senate) and Healthcare Freedom Act. Both facilitate transition from Diagram One to Diagram Two; both are waiting on terminal hold for Speaker Nancy Pelosi to bring them up for a vote. We must vote for leaders who will fight against bureaucrats, middlemen, and politicians and who will fight for us to have control of our medical decisions and dollars. It’s Medicare for All or Personalized Healthcare for you. Bureaucrats first or America First. President Trump has been doing this all along step by step through regulatory reform and Executive Orders, but he can’t complete the job without our votes, all the way down the ballot. He’s done so much almost single-handedly to drain the healthcare swamp. It’s time for us to help him wring the healthcare mop and finish the clean up.
Kristin S. Held, M.D.
Immediate Past President- Association of American Physicians and Surgeons